These burdens trickle down within teams, creating a stressful environment wherein team members must work with administrative tasks instead of focusing on patient care. Despite these pressures, physicians are also dedicated to providing quality care to their patients. 
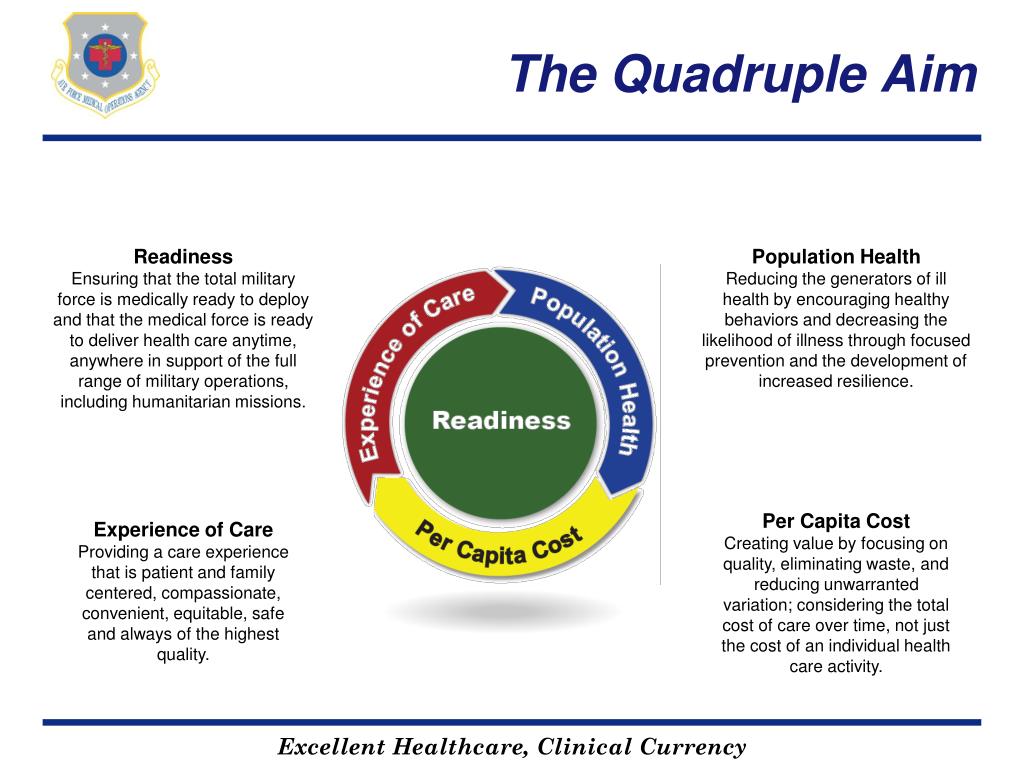
Many physicians spend hours of overtime completing EHR and other administrative tasks. These include expectations of physicians to generate wRVU by seeing more patients, suboptimal design of the EHR (electronic health record), shifting patient/consumer expectations of the provider-patient relationship, and a rapidly increasing alternative primary care sector, e.g., walk-in clinics, urgent care, concierge medicine, and online offerings. There are an increasing number of forces that create demands on providers’ performance and cognitive load. Thus, healthcare systems are facing 2 daunting yet seemingly opposed challenges: striving to achieve the goals proposed in the Quadruple Aim while increasing productivity. Most private insurers mimic this productivity-based reimbursement strategy. Reimbursement for care provided in the United States is based on productivity, i.e., work relative value units (wRVU), despite a shift towards value-based care by the Centers for Medicare and Medicaid Services. These foci are crucial for healthcare quality, yet healthcare systems must also consider other factors. These performance dimensions can be applied to far-reaching, crucial healthcare challenges, such as reducing the massive rates of burnout present in healthcare workers and combating rising healthcare costs. The framework encompasses reducing costs, improving population health and patient experience, with a new fourth domain: healthcare team well-being. In 2014, the Quadruple Aim-adapted from the widely-accepted Triple Aim -was suggested as a framework to optimize healthcare system performance.  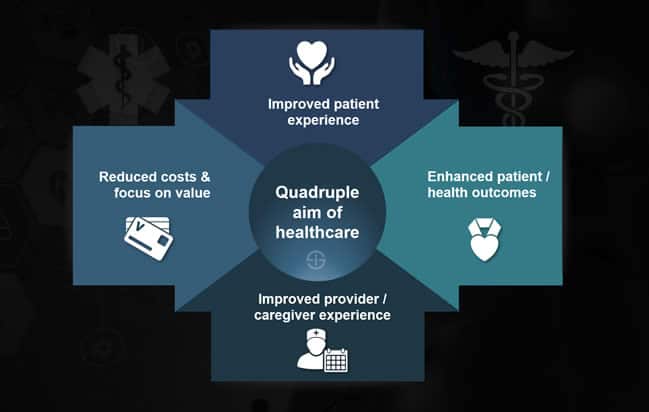
The Creative Commons Public Domain Dedication waiver ( ) applies to the data made available in this article, unless otherwise stated in a credit line to the data. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. 2021 56(Suppl 1):980-989.Open AccessThis article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. Emerging models of care for individuals with multiple chronic conditions. Centers for Disease Control and Prevention (CDC) website. Equitably addressing social determinants of health and chronic diseases. Population health strategies improve diabetes management. Care transitions improvement reduces 30-day all-cause readmissions saving nearly $2 million. Millions saved: complex care coordination reduces total cost of care. Transforming care for people with multiple chronic conditions: Agency for Healthcare Research and Quality's research agenda. Bierman AS, Wang J, O'Malley PG, Moss DK. AHRQ=Agency for Healthcare Research and Quality CDC=Centers for Disease Control and Prevention COPD=chronic obstructive pulmonary disease SDOH=social determinants of health.ġ.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
